No products in the basket.

This post originally appeared in ‘Julia’s dementia blog‘ in October 2017. We are really grateful to Julia for sharing her personal story with us and hope that it will help other carers in the same situation.
Take Care of Yourself First
Whether you care for a relative with dementia at home, visit them in a care home, or are a professional carer you need to be mindful of the potential toll on your own physical and mental health. It’s helpful advice that I dismissed. I suggest you don’t make the same mistake.
Carers taking care of ourselves

When I started caring for my mother, I was touched by kind messages from people I hardly knew telling me to take care of myself. I struggled to understand why there was so much emphasis on the carer. After all, it wasn’t me who was desperately anxious, confused and vulnerable as my mother was. And I already looked after myself.
Above all, I wasn’t the primary carer (at that time); my mum lived in a care home. I didn’t face that burden. I just visited my mum. I was almost embarrassed at the idea I might be at risk….
Three serious infections in two years
…And yet, perhaps it was no coincidence that since my mum’s problems started, I had three serious infections, two of which triggered sepsis, and resulted in hospital admissions. Normally, fit and healthy, my first infection was within a couple of weeks of my mother being admitted to hospital. For me a urinary infection, quickly moved to my kidney, and affected my liver. I was cared for in the same hospital at the same time as my mother, though she was in a locked ward.
My last infection was severe pneumonia which led to pleurisy, and infections of my gall bladder and liver. I remained in hospital for 10 days, until I could breathe enough oxygen into my lungs unaided. I think the trigger for my illnesses was the huge emotional turmoil of caring for someone you love, someone who is so deeply distressed.
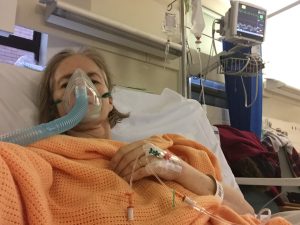
Feeling emotional and down
One weekend, I found myself feeling flat and weary during a visit with mum. I hadn’t intended to spend five hours with her that day, but I didn’t like to leave as she seemed particularly needy and helpless. That evening I had planned to restart a fitness class which I had neglected. I was looking forward to it, but while I was with mum, I started feeling physically tired and a little unwell. I talked myself out of the class, although it was probably the tonic I needed.
This ‘down’ feeling came from nowhere and sometimes took hold of my mood for several days at a time. It’s not unusual. Everybody feels blue from time to time. The problem was that someone I loved was living in a nightmare.
The cognitive impairment caused by the disease made it hard for mum to make sense of everyday things, her insecurities were amplified, her self-esteem assaulted, and she often ended up feeling scared and vulnerable. On top of that she was in a strange place, that because of dementia, never became familiar. As she often said to me “I am scared out of my pants”.
Physical and mental health toll
Caring for someone with dementia can have impacts you wouldn’t expect. “Carers of people with dementia have increased risk of developing dementia,” according to dementia care expert, Teepa Snow.
“Compared to non-caregivers, carers for people with dementia visited their GPs 50% more and took up to 86% more prescribed medications,” according to Alzheimer Scotland.
Family caregivers of people with dementia are “often called the invisible second patients”, according to an article in Dialogues, a clinical neuroscience magazine. “The effects of being a family caregiver, though sometimes positive, are generally negative, with high rates of burden and psychological morbidity as well as social isolation, physical ill-health, and financial hardship.”
A literature review on the topic concluded, “It appears that the majority of dementia caregivers are sufficiently disturbed to be of concern to the mental health professions.”
Reaction to emotional distress
Without the responsibility of managing mum’s daily needs, I didn’t face the 24-hour physical and practical job that some families do. The major impact for me was at an emotional level. I felt guilt and sadness. I was haunted by the thought she would be better off in her own home if only I was willing to support her. My sadness about her ongoing distress was at a deep and visceral level.
I was initially reluctant to connect my illnesses, with the situation my mother was in. Having subsequently learnt about the clear connection between mind and body, I think there is no getting around it. It is likely that my own emotions increased my susceptibility to illness.
So, although I already took good care of myself and my caring role at that time was minimal, I became more conscious of symptoms and moods, and more dedicated to preserving my physical and mental health. I learned to seek medical advice early if in any doubt at all. My persistence in getting medical attention during my third infection may well have saved my life. Not trusting my second diagnosis, I admitted myself to A&E where I was soon diagnosed with double pneumonia which quickly led to sepsis. In the UK, over a fifth of the 250,000 people who are affected by sepsis every year, die from the condition.
Take care of yourself
If your primary concern is your loved one, don’t forget you won’t be much use to them if you become ill. Teepa Snow, suggests you won’t be good company either, “If you’re in survival mode, you are not the kind of person that someone with dementia wants to be around!”
Even if you don’t think you are susceptible to physical or mental health strains it makes sense to be proactive. Alzheimer Scotland has put together a very useful guide for carers called ‘Looking After Yourself’ (PDF). I include the top tips here, though the whole document is well worth a read:
- Exercise: Keep up or take up exercise and outdoor walking, as far as possible. It helps you to stay healthy and relieve daily stress. You may even be able to do some activities with the person who has dementia. Exercise is also very good for people with dementia, as I highlight in this post about tackling anxiety and depression.
- Sleep: Regular sleep and rest are essential. If you don’t get enough rest it can lead to depression and affect your health. A leading neuroscientist recently highlighted a link between poor sleep and increased risk of developing dementia.
- Health: Watch out for signs of your own physical or mental distress. Keep an eye out for symptoms that may seem benign at first. Don’t be afraid to get them checked out with the doctor. If you find you’re not sleeping, or constantly feeling down go to your doctor.
- Relax: Try to take time out to do the things that you find relaxing such as getting a massage, doing yoga, or listening to calm music.
Breathe
Teepa Snow has advice about how to manage those stressful moments when you are with the person you care about, in the first of a great series of short videos for carers. Take “three deep cleansing breaths” when you find yourself becoming fraught or distraught. This is important to address our physiological reactions to pressure. When we start feeling stressed our bodies tense up and our breath becomes shallow. We breathe in, but not out, as we go into survival mode. This stops us getting enough oxygen into our brain, which affects the emotional control centre and the front part of the brain that helps us to make good decisions. This short little exercise that you can do again and again, helps you to take care of yourself, and enables you to take better care of your loved one. Watch the video. When my mother was feeling anxious, I led her through a version of this exercise too.
Julia Powell now runs mindfulness courses and coaching for carers and people living with dementia. Contact her at julia@juliapowell.co.uk to be added to her mailing list for upcoming courses.








